You Standardized the Platform. So Why Is Your Pathology Workflow Still Fragmented?
Many health systems today look standardized on the surface. Infrastructure is aligned. Transcription has been reduced or eliminated. Speech has been...

In today’s digital world, electronic health records (EHRs) are an extension of what we expect in our everyday lives: information readily available at our fingertips. No longer do patients need to call the doctor’s office to double check the bloodwork or biopsy results they forgot to jot down during their appointments. That information is easily accessible in one location online, with the EHR serving as a central repository for all patient encounters with primary care physicians, specialists, nurses, lab technicians, and other clinicians.
Beyond empowering patients to take control of their health, a well-managed EHR system offers plenty of benefits for physicians, staff, and hospitals, including better efficiency, improved patient outcomes, and cost savings.
But with any technology, there’s always room for improvement. In an editorial in the Journal of General Internal Medicine, Regenstrief Institute research scientist Dr. Michael Weiner highlights some shortcomings of EHRs that are challenging for care providers and potentially dangerous for patients.

Dr. Michael Weiner, image courtesy of Regenstrief Institute
“What I encounter much too often is that key pieces of the patient’s record are in the wrong place or embedded so deeply in the EHR that they are hard to locate or may not even have been documented,” Dr. Weiner says in his editorial, titled “Forced Inefficiencies of the Electronic Health Record.”
In fact, Dr. Weiner claims, electronic health records have continued to enable inconsistency and potentially undesirable variation in documentation and, sometimes, even the clinical care associated with it.
Dr. Weiner proposes more than a dozen specific principles to improve EHRs, to the benefit of both clinicians and their patients. He challenges EHR vendors, health systems, doctors, nurses, and other front-line professionals to fight inefficiencies and improve the function of the EHR. Many of his recommendations target EHR vendors and their product designs, while others are directed at users who work in healthcare settings.
A patient's pathology report is an exceedingly important part of his or her EHR. Often called the "doctor's doctor," the pathologist identifies disease and shapes other physicians' treatment plans. Many times, patients can view their lab results and read their own pathology reports in the EHR.
As a vendor providing speech recognition technology and reporting tools for pathology professionals, Voicebrook understands the importance of consistency and efficiency when it comes to medical records and reports. The VoiceOver PRO reporting tool integrates directly with Anatomic Pathology (AP) systems to allow pathology staff to build the highest-quality reports faster and with fewer inputs. That means pathology results will be available in the patient’s EHR in a timelier manner, with a higher level of accuracy.
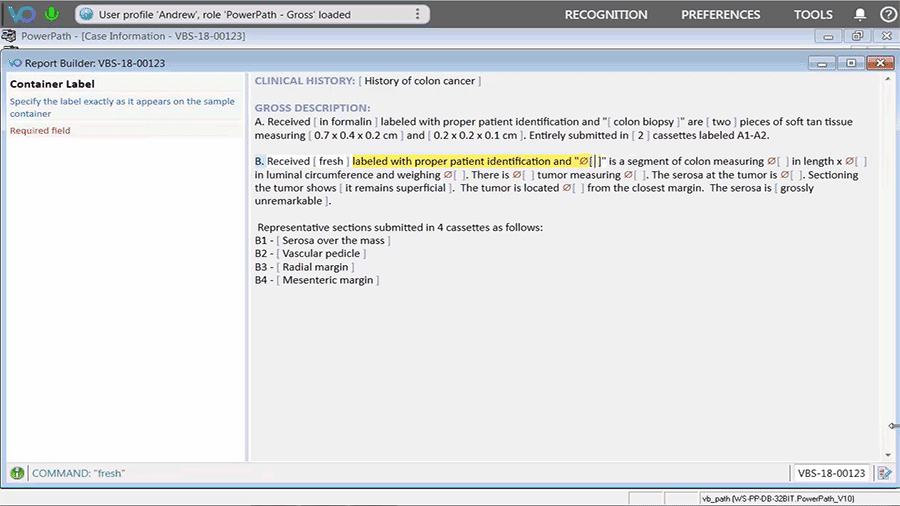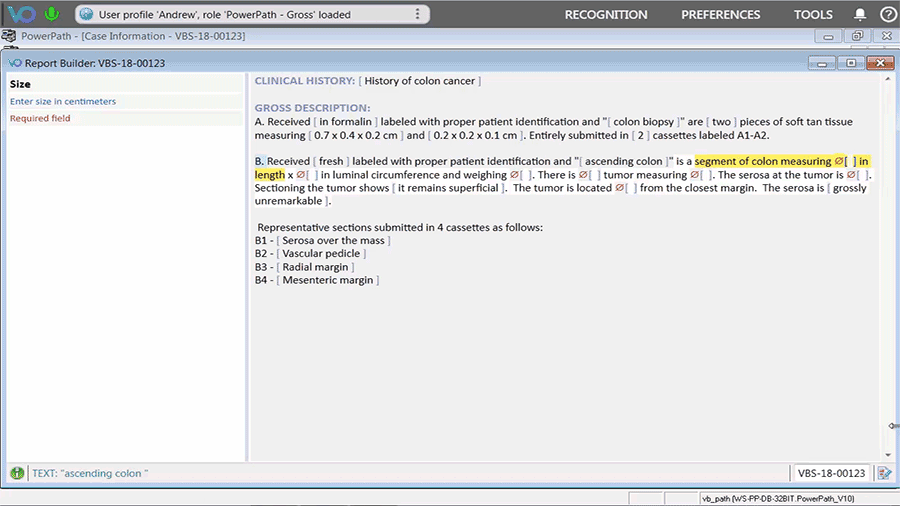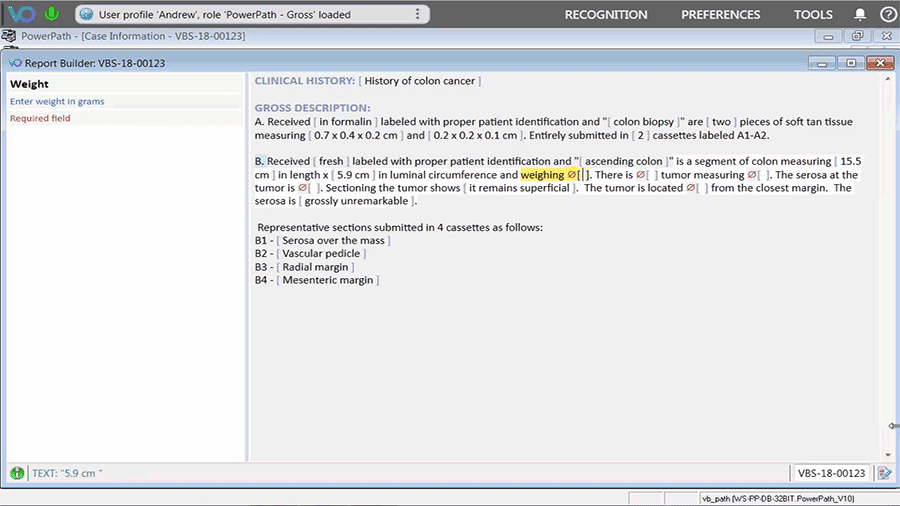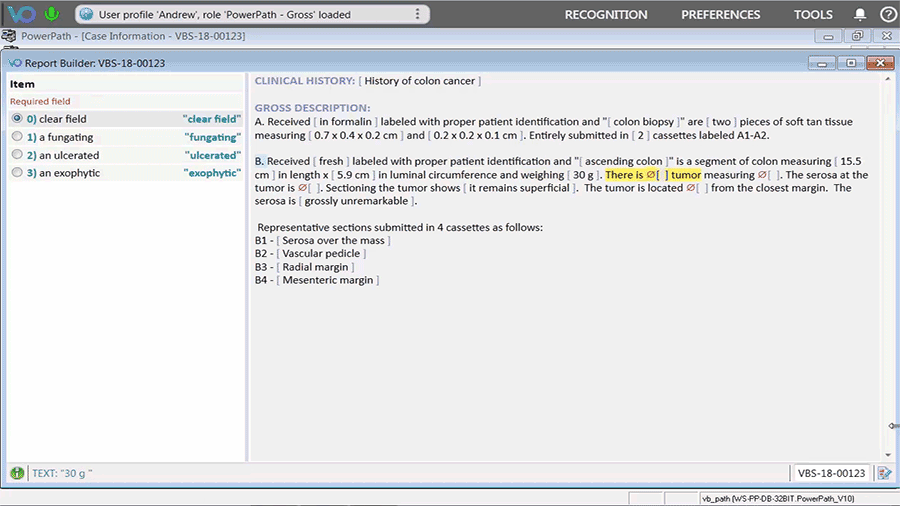
One of Dr. Weiner’s suggestions for improving EHRs is to use strategies that are thought or shown to save time, such as minimizing the number of clicks, providing options for keyboard shortcuts, and making touchscreens available for selected functions. VoiceOver PRO offers multiple dictation workflows and configurations to fit the needs of individual users. The ability to customize templates and use an assortment of input devices improves quality, speed, and productivity while reducing costs.
Dr. Weiner notes that, when it comes to medical records, “I still want my voice, that part of the record that tells other people what I think the problem is, and what should be done about it.” That’s what truly makes the difference in patient care, and it’s why Voicebrook is in business. We want to help you focus on your patient’s report, not your technology. The right tools make all the difference.


Many health systems today look standardized on the surface. Infrastructure is aligned. Transcription has been reduced or eliminated. Speech has been...
.png)
When Stamford Health made the enterprise-wide shift to Epic, their pathology department faced a familiar dilemma: would the new system support their...

Medical laboratories are intrinsic to the ultimate well-being of patients everywhere. That's never been more evident than now, during our current...